Paying for curative gene therapies: potential, barriers and healthcare reforms for risk-sharing between payers and industry in a multi-payer healthcare system
For further discussion about the analysis of risk sharing models for costly gene therapies, we would like to invite you to view our poster presentation at the Virtual ISPOR Europe 2020 conference which takes place from the 16th until the 19th of November.
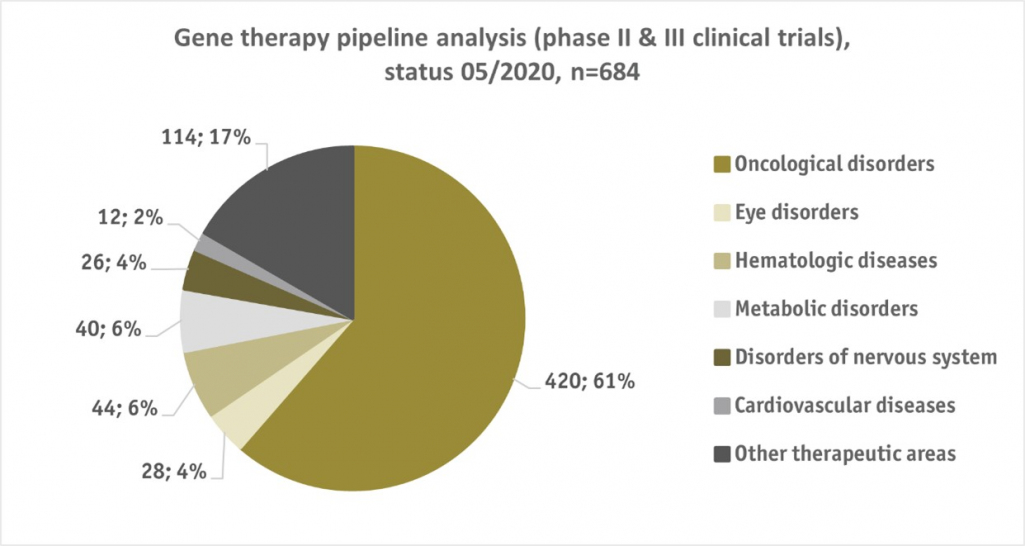
Gene therapies promise revolutionary benefits for patients and healthcare systems, with a full clinical trial pipeline indicating a further paradigm shift in medicine, but the novel logic of a one-off, potential cure creates challenges for both healthcare payers and manufacturers with respect to the upfront payment logic. To date, a total of 684 phase 2-3 studies are in the clinical gene therapy pipeline, with the majority of 61% relating to the oncological field. In addition, new breakthroughs in highly prevalent and thus financially burdensome therapeutic areas such as metabolic diseases and cardiology are likely in the next few years.
To secure affordability for healthcare systems and to share the risk of uncertain long-term efficacy and safety, risk-sharing models such as pay for performance are increasingly adopted in reimbursement negotiations between pharmaceutical manufacturers and payers. P4P models include the real-life performance in the level of remuneration, i.e. the outcome in previously determined patient relevant endpoints several months after application of the pharmaceutical product. However, barriers intrinsic to a multi-payer healthcare system impede the effective use of P4P for ATMPs and no universal one-size-fits-all approach will work in practical use. These barriers include the definition and measurement of "success" and a sufficient access to medical data in order to quantify the prespecified success. Another hurdle is the high administrative burden for both parties to negotiate and manage the risk-sharing deals. Centralized risk-sharing agreements are considered as a potential remedy, but face obstacles in a multi-payer system with statutory health insurances (SHIs) covering highly divergent patient and financial structures.
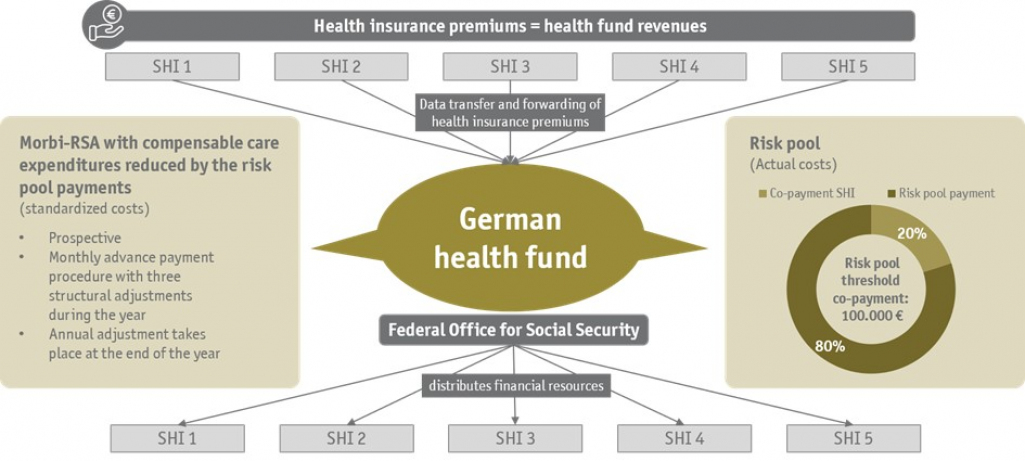
To compensate unequal financial burdens between funds, a risk pool will be introduced in Germany in 2021, which will collectivize the expenses of high cost patients between SHIs. However, the risk pool entails new barriers for P4P models, especially regarding installment payment plans
To gain more information on this topic, we would like to invite you to take part in the online discussion taking place on November 18, 2020 between 3:00 – 4:30 pm at the Virtual ISPOR Europe 2020. Alternatively, please click here to view our poster presentation at this year's virtual ISPOR Europe.